Pancreatic cancer is considered particularly dangerous because it is often diagnosed late and metastasizes early. Learn more in this article.
In Switzerland, approximately 1,600 individuals, primarily older adults, are diagnosed with pancreatic cancer annually. This malignancy poses a significant medical challenge due to its aggressive nature and the difficulty of early detection, resulting in a tragically low survival rate.
The Challenge of Late Diagnosis
Pancreatic cancer often remains undetected until it reaches advanced stages. This is largely because early symptoms are vague and easily confused with other, less serious conditions. Moreover, the pancreas's deep location within the abdomen makes early detection difficult, especially as routine screening is not widely implemented. The tumor's rapid growth further compounds this issue.
Sadly, only about 12% of patients survive five years post-diagnosis. This stark statistic reflects the fact that the cancer is frequently discovered after it has metastasized, spreading to vital organs like the duodenum, gallbladder, spleen, or peritoneum.
The combination of late-stage diagnosis and limited effective treatment options makes pancreatic cancer one of the most lethal forms of cancer.
What is Pancreatic Cancer?
Pancreatic cancer, also known as pancreatic carcinoma, is a malignant tumor of the pancreas. It is considered particularly dangerous because it is often detected late and tends to form metastases early, spreading to other organs.
The pancreas plays crucial roles in digestion and blood sugar regulation, both of which are severely compromised by pancreatic cancer:
- Exocrine Function: It produces digestive enzymes essential for breaking down food in the small intestine.
- Endocrine Function: As an endocrine gland, it produces hormones, particularly insulin, which is responsible for the uptake of sugar from the blood into cells and the regulation of blood sugar levels. Disruption of this function can lead to diabetes mellitus.
Why Is Pancreatic Cancer Often Not Curable?
Pancreatic cancer is known for its high mortality rate and the challenges it poses for early detection and treatment. Here are the key reasons why pancreatic cancer is often not curable:
1. No Standard Screening Test
Unlike other cancers, there is no established screening test for pancreatic cancer. Even if a highly accurate test were developed, there would still be a risk of too many false-positive results. These could lead to unnecessary invasive tests and treatments. The German Cancer Society (DKG) stresses the urgent need for improvements in early detection methods to better identify the disease at its earliest stages.
2. Location of the Pancreas
The pancreas is located deep within the abdominal cavity, making it difficult to access directly for examination, unlike other organs such as the intestines during a colonoscopy. This anatomical positioning means that early changes in the pancreas are often not detectable. Moreover, the pancreas is situated near critical blood vessels, such as the abdominal aorta and the inferior vena cava. As a result, surgery to remove pancreatic tumors is often complex and carries significant risk.
3. Early Metastasis
Pancreatic cancer is known for its aggressive nature and its tendency to spread (metastasize) to other organs at an early stage. In contrast, other cancers, such as colon cancer, may take up to 10 years for a precursor lesion to evolve into an invasive tumor. The rapid spread of pancreatic cancer makes it difficult to treat effectively once detected.
4. No Symptoms in the Early Stage
In the early stages of pancreatic cancer, patients often experience no symptoms or only vague, nonspecific symptoms, such as abdominal pain or digestive issues. These symptoms are easily attributed to less serious conditions, which can delay the diagnosis. By the time a diagnosis is made, the cancer is often already in an advanced stage, making it much more difficult to treat.
What Symptoms Occur with Pancreatic Cancer?
- Pain in the Upper Abdomen or Radiating to the Back
This pain may be dull or sharp and often worsens after eating or when lying down. - Jaundice
Tumors in the head of the pancreas can block the pancreatic duct, leading to jaundice, as the bile duct becomes obstructed, thereby hindering bile flow. - Loss of Appetite and Weight Loss
The tumor can impair digestion, causing nausea, vomiting, and altered satiety, leading to unintended weight loss. - Fatty Stools
Due to impaired fat digestion, the stool may become light, fatty, and foul-smelling. - New-Onset Diabetes
The tumor can interfere with insulin production, leading to high blood sugar levels. When diabetes is caused by a pancreatic disease, it is referred to as Type 3c diabetes mellitus. Around 5-10% of diabetics in industrialized nations have this form of diabetes. - Fatigue and Weakness
Due to the illness and disrupted digestion, a general feeling of weakness and fatigue can occur. The exhaustion experienced by cancer patients is disproportionate to the physical activity they engage in.
What Are the Risk Factors and Causes of Pancreatic Cancer?
The exact causes of pancreatic cancer are not yet fully understood. However, several factors can increase the risk of developing this type of cancer.
The most important risk factors include:
- Smoking
Smoking is the greatest risk factor for pancreatic cancer. Smokers have approximately twice the risk of developing pancreatic cancer compared to non-smokers. Studies show that smokers have an 80% higher risk of developing pancreatic carcinoma. Smoking doubles the risk because carcinogenic substances in tobacco can directly damage the pancreas. - Alcohol Consumption
Regular and excessive alcohol consumption also increases the risk. People who consume more than 30 grams of alcohol daily (equivalent to two bottles of beer or three glasses of wine) have a moderate risk of developing pancreatic cancer. - Overweight and Obesity
People with significant overweight also have an increased risk. A 2011 study found that approximately 12% of pancreatic carcinomas in the UK were linked to overweight or obesity. - Type 2 Diabetes
Diabetes can either be a risk factor or a symptom of pancreatic cancer. Pancreatic cancer is 1.5 to 2 times more common in people with long-term diabetes (over 3 years) compared to those without diabetes. - Chronic Pancreatitis
People with chronic pancreatitis (inflammation of the pancreas) have an increased risk of pancreatic cancer. Studies suggest that the risk may be two to three times higher compared to the general population. - Family History
If close relatives (parents, siblings, children) have had pancreatic cancer, there is about an 8% risk of also developing the disease. - Genetic Factors
Certain genetic mutations can increase the risk. It is suspected that BRCA1 mutations may be linked to a higher risk of pancreatic adenocarcinoma. Studies on families with BRCA1 mutations, where early breast and/or ovarian cancer has been identified, suggest that the risk of pancreatic cancer in BRCA1 carriers is 2-3 times higher than in the general population. - Age
The risk increases with age. Most people are diagnosed after the age of 60, with the average age of diagnosis being 76 for women and 71 for men. As the population ages, the statistical likelihood of developing pancreatic cancer also increases.
How Does Pancreatic Cancer Typically Progress?
The course of pancreatic cancer is often aggressive and characterized by the following features:
Early Stage:
- Few to No Symptoms: In the early stages, pancreatic cancer often causes little or no symptoms, making early diagnosis difficult.
- Rapid Growth: The tumor often grows quickly and can invade surrounding tissues and organs, such as the duodenum, stomach, liver, or bile ducts, at an early stage.
- Metastasis: Pancreatic cancer tends to form metastases early, particularly in the liver, lymph nodes, and lungs.
Advanced Stages:
- Increasing Symptoms: As the disease progresses, typical symptoms such as upper abdominal or back pain, jaundice, weight loss, and digestive disturbances emerge.
- Treatment Resistance: Pancreatic cancer often responds poorly to chemotherapy and radiation therapy, making treatment more challenging.
- Complications: The tumor can lead to complications such as bowel obstruction, bleeding, or infections.
Prognosis:
- Poor Overall Prognosis: Pancreatic cancer has one of the worst prognoses among all cancers. The 5-year survival rate is about 10% overall.
- Impact of Stage: The prognosis depends heavily on the stage of the disease at diagnosis. Early diagnosis and operable cases offer a better prognosis.
- Palliative Care: In advanced stages, treatment focuses on alleviating symptoms and improving the quality of life.
How is Pancreatic Cancer Diagnosed?
The diagnosis of pancreatic cancer typically involves several steps, including both imaging techniques and laboratory tests.
1. Medical History and Physical Examination:
The doctor will first gather the patient's medical history, asking about overall health, pre-existing conditions, potential risk factors, and any current symptoms. A thorough physical examination will then be conducted, with particular attention to palpating the abdomen to check for signs such as jaundice or an enlarged liver.
2. Imaging Techniques and Further Tests:
- Ultrasound: An abdominal ultrasound (sonography) can provide initial indications of a tumor in the pancreas. Sometimes, a specialized form of ultrasound, called endosonography, is used. This involves inserting a small ultrasound probe through a tube into the gastrointestinal tract to examine the pancreas more closely.
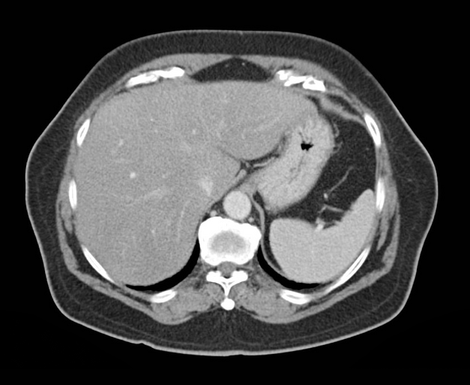
- Computed Tomography (CT): A CT scan provides detailed images of the pancreas and surrounding organs. It can help determine the size and location of the tumor and whether it has spread to other organs.
- Magnetic Resonance Imaging (MRI): An MRI also produces detailed images of the pancreas and is particularly useful for assessing the bile ducts and blood vessels near the tumor.
- Positron Emission Tomography (PET): A PET scan can help identify active cancer cells in the body, even if they are very small or located in other organs.
- Laparoscopy: This procedure allows for direct visual examination of the abdominal cavity and the surface of the liver. It can detect even small metastases (micrometastases) that may not be visible in imaging tests like CT or MRI. The presence of such metastases can affect the decision about the operability of the tumor, as it may indicate advanced disease.
3. Laboratory Tests:
- Blood Tests: Certain blood values, such as tumor markers CA 19-9 or CEA, may be elevated, but they are not specific to pancreatic cancer and should always be used alongside other diagnostic tests. CA 19-9 is a tumor marker used to monitor and assess the response to therapy in pancreatic cancer, but it is unspecific, as it can also be elevated in other conditions such as gallbladder inflammation, pancreatitis, or liver cirrhosis. Therefore, it is not suitable for early detection.
- Tissue Sample (Biopsy): A tissue sample, taken under ultrasound or CT guidance, allows for microscopic examination of the tissue and provides a definitive diagnosis of pancreatic cancer.
4. Additional Tests:
- ERCP (Endoscopic Retrograde Cholangiopancreatography): In this procedure, an endoscope is inserted through the mouth into the duodenum to visualize the bile ducts and pancreatic duct, and if necessary, obtain a tissue sample.
- Genetic Testing: If there is suspicion of hereditary predisposition, genetic tests may be conducted to detect inherited mutations. This includes genes such as BRCA 1 and BRCA 2 or FAP.
Typically, several imaging techniques are combined to get the most accurate picture of the disease. A definitive diagnosis of pancreatic cancer requires a tissue sample (biopsy).
How is Pancreatic Cancer Treated?
Surgery:
Surgery to remove the tumor is the only potentially curative treatment option for pancreatic cancer. However, this option is realistic for only about 20-30% of patients, as the tumor is often already advanced or inoperable. Surgeries on the pancreas, whether involving the head or tail of the pancreas, are considered extremely demanding and complex. Dr. Wolfgang Jungblut, a specialist in general surgery, vascular surgery, and visceral surgery, emphasizes the importance of thorough exploration before surgery to determine feasibility and the precise approach. The surgery itself can take 3-4 hours or longer.
Chemotherapy:
If the tumor has already reached or encased blood vessels, chemotherapy is administered before surgery. This so-called neoadjuvant chemotherapy aims to shrink the tumor and make the surgery safer by reducing the risk of complications. The chemotherapy drugs work by killing cancer cells or inhibiting their growth throughout the body. In addition to being used before surgery (neoadjuvant), they can also be used after surgery (adjuvant) to eliminate any remaining cancer cells. In advanced cancer, when surgery is no longer possible, chemotherapy can also serve as the primary treatment to slow down tumor growth and relieve symptoms.
Radiotherapy:
High-energy radiation is used to destroy cancer cells. It may be used before or after surgery, or in combination with chemotherapy.
Palliative Care:
When a cure is not possible, treatment focuses on alleviating symptoms, improving quality of life, and extending survival.
What is the Life Expectancy for Pancreatic Cancer?
The life expectancy for pancreatic cancer strongly depends on the stage of the disease at the time of diagnosis. Unfortunately, the chances of curing this type of cancer are relatively low. The 5-year survival rate, meaning the percentage of patients who are still alive five years after diagnosis, is about 9-13% for pancreatic cancer overall.
When diagnosed at an early stage, followed by prompt surgery and chemotherapy under the care of specialists in gastroenterology and oncology, cancer patients have a higher chance of recovery.
Conclusion: Surgery Only Possible for a Small Portion of Patients
Pancreatic cancer, also known as pancreatic carcinoma, is an aggressive form of cancer with a low survival rate. Late detection, rapid tumor growth, and early metastasis make treatment challenging.
Although surgery is the only potentially curative option, it is only possible for a small portion of patients. Chemotherapy, radiation therapy, and palliative care can slow disease progression and improve quality of life, but the overall prognosis remains poor.
Since pancreatic cancer is often asymptomatic in its early stages and there is no specific screening, the diagnosis is often made very late, negatively impacting the chances of a cure.
Early diagnoses through imaging techniques such as an MRI scan are therefore crucial. In addition to the pancreas, an MRI full-body scan can examine many other organs and tissues to detect changes at an early stage.