False positive or false negative MRI results can have serious consequences. Learn in this article how MRI misdiagnoses occur and what steps we take to prevent them.
Misdiagnoses in Magnetic Resonance Imaging (MRI) can never be completely ruled out. According to a study by the Radiological Society of North America, diagnostic errors in imaging procedures like MRI, CT, or X-rays occur in about 3-5% of cases worldwide. This includes both false positive and false negative results across all radiology imaging methods, such as MRI, computed tomography (CT), X-rays, and ultrasound.
What Is an MRI Misdiagnosis?
An MRI misdiagnosis occurs when the images are not correctly interpreted. This can happen in the following ways:
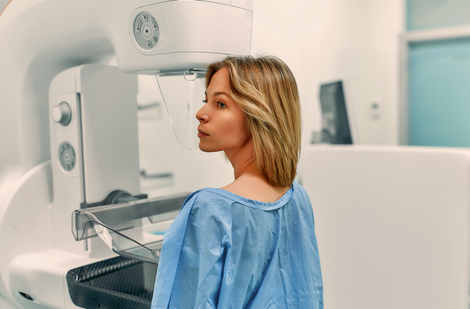
- False Positive: A normal finding is incorrectly interpreted as abnormal. For example, a breast cancer screening study showed false-positive results for breast cancer in 83% of cases for 465 women, which had to be clarified through additional tests.
- False Negative: An abnormal finding goes undetected. This can occur even with MRI’s high sensitivity, especially with small tumors or specific lesions.
- Diagnostic Confusion: An abnormal finding is mistaken for another condition, such as inflammatory processes that may produce signals similar to tumors.
- Delayed Diagnosis: A correct diagnosis is made too late, worsening treatment outcomes.
- Insufficient Patient Information: If results are not clearly communicated, patients may not be able to make informed decisions.
Why Do MRI Misdiagnoses Occur?
There are several reasons why MRI misdiagnoses can happen.
Technical issues can certainly affect image quality, but this is rare.
Sometimes patient movements during the scan can cause inaccuracies, or there may be other patient-related limitations. For example, a necessary contrast agent cannot be used due to gadolinium intolerance. Additionally, implants like pacemakers and other metal objects in the body pose significant challenges for MRI scanners, which rely on strong magnetic fields. If an MRI is possible despite such metal objects, they can distort or obscure the images, complicating precise interpretation.
It is also possible that the radiologist lacks the experience to select the appropriate sequence or correctly assess complex findings. However, in Switzerland, where training and practice standards are high compared to other countries, and with strong emphasis on quality assurance and continuous education from the Swiss Society of Radiology (SGR / SSR), this is not a significant concern.
How Likely Are MRI Misdiagnoses?
Specific statistics focusing exclusively on MRI misdiagnoses are not currently available. Global estimates suggest that the error rate for radiology imaging procedures, including MRI, is about 3-5% per year. The rate for MRI could be lower, but certain types of scans, like breast cancer screenings, have shown much higher error rates — one study found an 83% false-positive rate.
In Switzerland, according to the Foederatio Medicorum Helveticorum (FMH), only 60 expert opinions on possible breaches of duty of care in radiology were filed over 40 years, with 16 cases proving actual violations.
Consequences of MRI Misdiagnoses
MRI misdiagnoses do not always lead to treatment errors, but they can have significant negative effects, even if corrected later. Especially in sensitive exams like full-body MRIs, follow-up investigations are common to minimize risks. False positives can trigger unnecessary tests and treatments, leading to wasted time, extra costs, and psychological stress due to the suspicion of serious illness. Unnecessary treatments may also pose risks, while false negatives delay timely treatment and worsen the prognosis.
How Does Aeon Minimize the Risk of Misdiagnoses?
At Aeon, we reduce the risk of misdiagnoses through cutting-edge technology, standardized processes, and close collaboration between specialists.
Would you like to learn more about the benefits of an MRI scan for you and your health? Then schedule a free consultation and get the information you need.